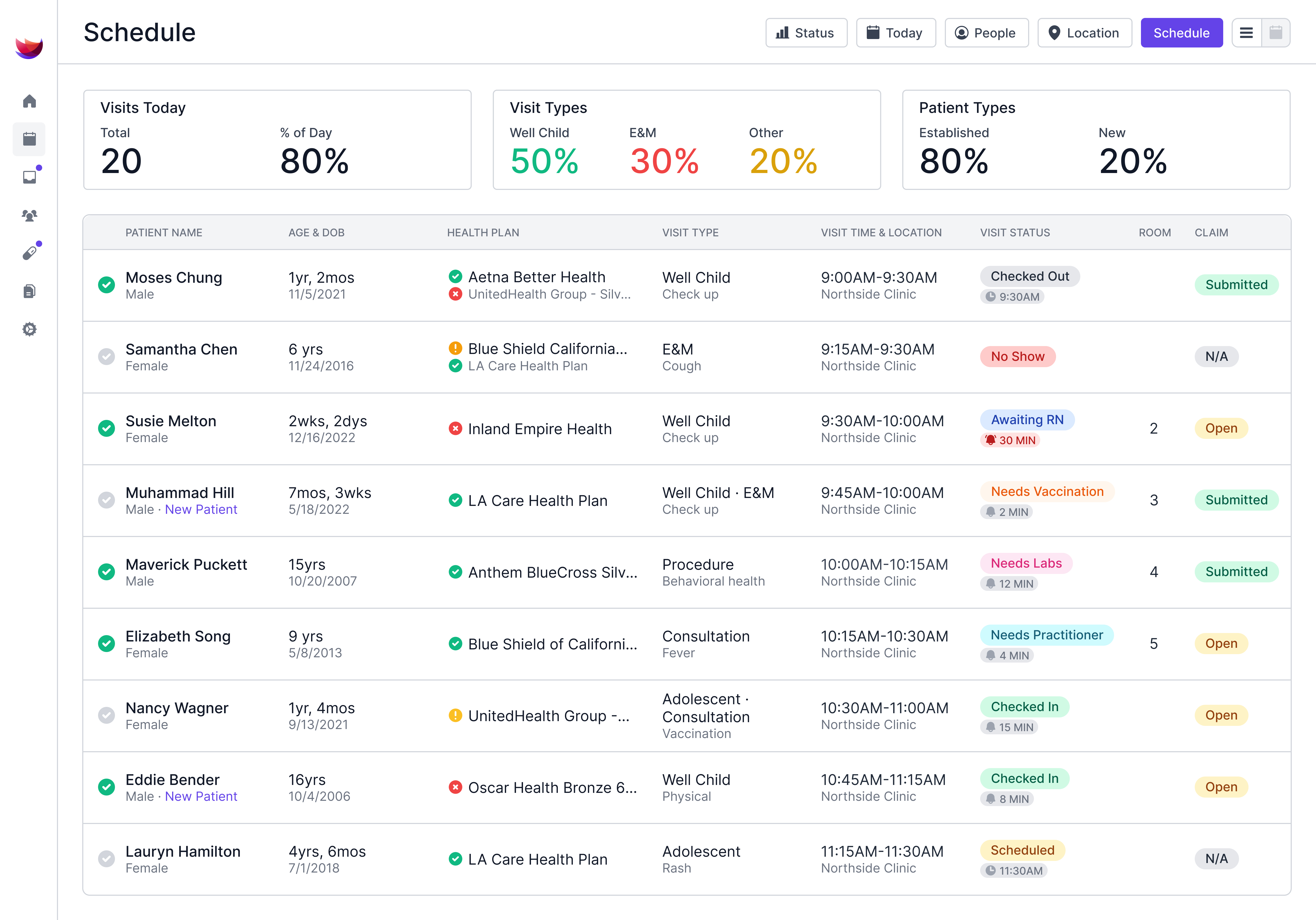
Your pediatric office workflow shapes everything from how quickly a family gets seen to how much time your team spends finishing notes after hours, and clinics that get it right see real improvements in both care quality and staff satisfaction.
Here are practical examples from real pediatric practices, plus what you can do to make them work for your clinic.
What Does an Effective Pediatric Office Workflow Look Like?
An effective pediatric office workflow moves patients smoothly from check-in to checkout, keeps staff roles clearly defined, and uses documentation tools that support clinical work rather than slow it down.
In practice, that breaks down into four main zones: front office, clinical intake, provider visit, and checkout/billing. When each zone has clear ownership and a consistent handoff process, bottlenecks become much easier to spot and fix.
The American Academy of Pediatrics (AAP) recommends starting with the patient's experience. Shadow a visit from the family's point of view, note where time is lost, then review the full flow as a team before making any changes.
Make one change at a time, with evaluation in between. Clinics that try to fix everything at once could find themselves creating new problems before the original ones are resolved.
Common Pediatric Office Workflow Problems (and What To Do About Them)
Some of the most common pediatric office workflow problems are documentation overload, poor scheduling structure, and unclear role assignment. They also tend to compound each other.
Documentation Overload
Research shows that many outpatient physicians spend up to twice as much time interacting with the electronic medical record (EMR) as they do with patients.
In pediatric primary care, that translates to notes finished at night, rushed visits, and staff who feel like data-entry clerks rather than care providers.
Clinics that pre-chart before patients arrive see significant time savings. Pulling up the chart, reviewing growth trends, flagging overdue vaccines, and noting outstanding referrals before the family walks in cuts in-room documentation time considerably.
Pairing that with visit templates built around your most common visit types (well child checks, sick visits, behavioral health follow-ups) reduces documentation load further.
The AAP also recommends assigning front desk staff to verify insurance and complete form review before the visit starts, so clinical staff aren't handling admin tasks mid-flow.
Scheduling Structure
Scheduling mismatches are one of the quickest ways to throw off clinic flow. Overscheduling creates wait times that frustrate families. Underscheduling leaves revenue on the table.
Effective practices intentionally segment their schedules: blocks for well visits (longer, predictable), blocks for acute visits (shorter, variable), and buffer slots throughout the day for same-day add-ons.
That structure means a sick visit at 10 AM doesn't turn into a 45-minute delay for a 4-year-old's well check at 10:30.
Some clinics also use their EMR's tracking view to monitor real-time patient location during the day, which lets medical assistants (MAs) redirect flow before congestion builds rather than reacting to it afterward.
Unclear Role Assignment
When roles aren't clearly defined, tasks fall through the gaps or pile up on the wrong people.
MAs and registered nurses (RNs) are most effective when they're doing the work they're trained to do.
In high-performing pediatric practices, MAs handle exam room prep, vital signs, vaccine administration, and gathering clinical info like lab results and prior records. RNs manage clinical triage, patient education, and care coordination. Physicians and nurse practitioners (NPs) focus on the visit itself.
The AAP frames MAs and RNs as flow managers rather than support staff. Giving clinical staff clear ownership over their segment of the workflow tends to produce better outcomes and higher team satisfaction.
How EMR Design Affects Pediatric Workflow
Pediatric practices have unique documentation needs: growth charts, developmental screening, immunization tracking, and daycare or school forms. Generic systems aren't built for any of that, and clinicians end up spending more time working around the software than actually using it.
When clinicians are stuck using tools that weren't built for their workflow, it shows up in the data. In some pediatric settings, 44% of charts weren't being completed until after clinic hours, a clear sign that the system was working against the team.
Get the EMR right, and the opposite happens. Practices that use pediatric-specific visit templates, automated recall reporting, and streamlined documentation can add capacity without adding staff. Better scheduling and tracking tools alone can meaningfully increase monthly visit volume.
The features that make the biggest difference in pediatric office workflow:
- Pre-visit chart prep tools that surface overdue items before the appointment, so nothing gets missed mid-visit
- Pediatric visit templates that reflect the real structure of well child and sick visits, not generic adult workflows
- Tracking views that let staff see patient location and status across the clinic in real time
- Automated communications for appointment reminders and post-visit follow-ups
- School, daycare, and camp form automation, which cuts the admin burden for front office staff
- Recall reporting to proactively identify patients due for wellness visits or immunizations
Practical Workflow Improvements for Pediatric Clinics
Here are some specific changes worth considering for your pediatric office workflow.
Pre-Visit Preparation Protocols
Assigning one MA per provider to complete a pre-visit checklist 24 hours before each appointment (chart review, insurance verification, outstanding lab flag, vaccine due check) can reduce visit duration and make same-day cancellations easier to backfill.
Role-Specific Task Ownership
Checkout delays often happen because the wrong people are handling billing clarifications. Assigning a dedicated billing liaison and giving them the right EMR access can solve that problem and improve co-payment collection rates.
Same-Day Sick Visit Blocks
Reserving two to three same-day slots per provider per session gives families timely access without overloading a full schedule. It can also reduce no-show rates on planned appointments, because families no longer feel like they need to hold a slot just in case.
Post-Visit Follow-Up Automation
Setting up automated follow-up appointments that prompt your staff to schedule a patient or enable patients to self-schedule after sick visits, well child checks, or chronic disease management appointments can cut inbound call volumes and help families stay engaged with their care plans.
How Develo Supports Better Pediatric Office Workflow
Documentation overload, scheduling gaps, and unclear role ownership are workflow problems. But they're also people problems that push good clinicians and staff toward burnout. Most of the time, they trace back to a system that was never designed for pediatrics in the first place.
Develo is a modern EMR built exclusively for independent pediatric practices, designed around the workflows, family structures, and clinical needs specific to pediatrics.
Here's what that looks like in practice:
- AI Scribe automatically captures the patient encounter, so providers can finish the visit with documentation already completed rather than carrying it home.
- Sophisticated visit templates for well child checks, sick visits, and other common appointment types, with relevant orders, diagnoses, and billing codes built in.
- Automated charge capture that applies pediatric-specific billing codes based on documentation, reducing manual biller workload and bringing down denial rates.
- Age-appropriate clinical screeners that auto-populate ahead of each visit based on the patient's age, covering developmental, behavioral health, and autism screening without any manual setup.
- Family portal with digital intake so families complete forms before they arrive, front desk staff isn't transcribing paper, and check-in actually runs on time.
- Automated recall and follow-up that keeps patients coming back for wellness visits and follow-up care without your team having to chase anyone down.
- Native family relationship management for blended families, multiple guardians, and siblings is handled cleanly within the system rather than through workarounds.
- Integration with all 50 state immunization registries for accurate, compliant vaccine records without manual reporting.
Develo brings scheduling, documentation, billing, and family engagement together in one platform, so your team spends less time managing systems and more time on patients.
Book a free demo to see how Develo streamlines your pediatric office workflow, from check-in through to claim submission.
Frequently Asked Questions
What Is a Pediatric Office Workflow?
A pediatric office workflow is the sequence of steps that moves a family through a clinic visit, from scheduling and check-in through the provider encounter, checkout, and follow-up.
An optimized workflow keeps each step clearly owned, reduces wait times, and lets clinical staff focus on patient care rather than admin.
What Are the Most Common Pediatric Office Workflow Bottlenecks?
The most common pediatric office workflow bottlenecks are documentation overload, scheduling mismatches, and unclear role assignment. They tend to compound each other, so addressing one usually reduces pressure on the others.
How Can an EMR Improve Pediatric Office Workflow?
An EMR improves pediatric office workflow by automating routine tasks, centralizing clinical and billing data, and reducing manual work across the team. Pediatric-specific features like immunization tracking, growth charts, and digital intake make the biggest difference for independent pediatric practices.
How Do You Reduce Documentation Burden in a Pediatric Clinic?
You reduce documentation burden in a pediatric clinic by pre-charting before visits, using visit templates, and choosing an EMR built around pediatric workflows rather than adapted from a generic system.
Research shows that physicians who spend excessive time on documentation outside of work hours are significantly more likely to experience burnout, making this a staffing and retention issue as much as an operational one.
How Should a Pediatric Clinic Handle Same-Day Sick Visits Without Disrupting Scheduled Appointments?
A pediatric clinic should handle same-day sick visits by building protected buffer slots into each provider's daily schedule rather than squeezing add-ons into existing appointment blocks. Reserving two to three same-day slots per provider per session gives families timely access while keeping the rest of the schedule intact.


.avif)

.jpg)

%20(1).jpg)
.avif)
.jpg)