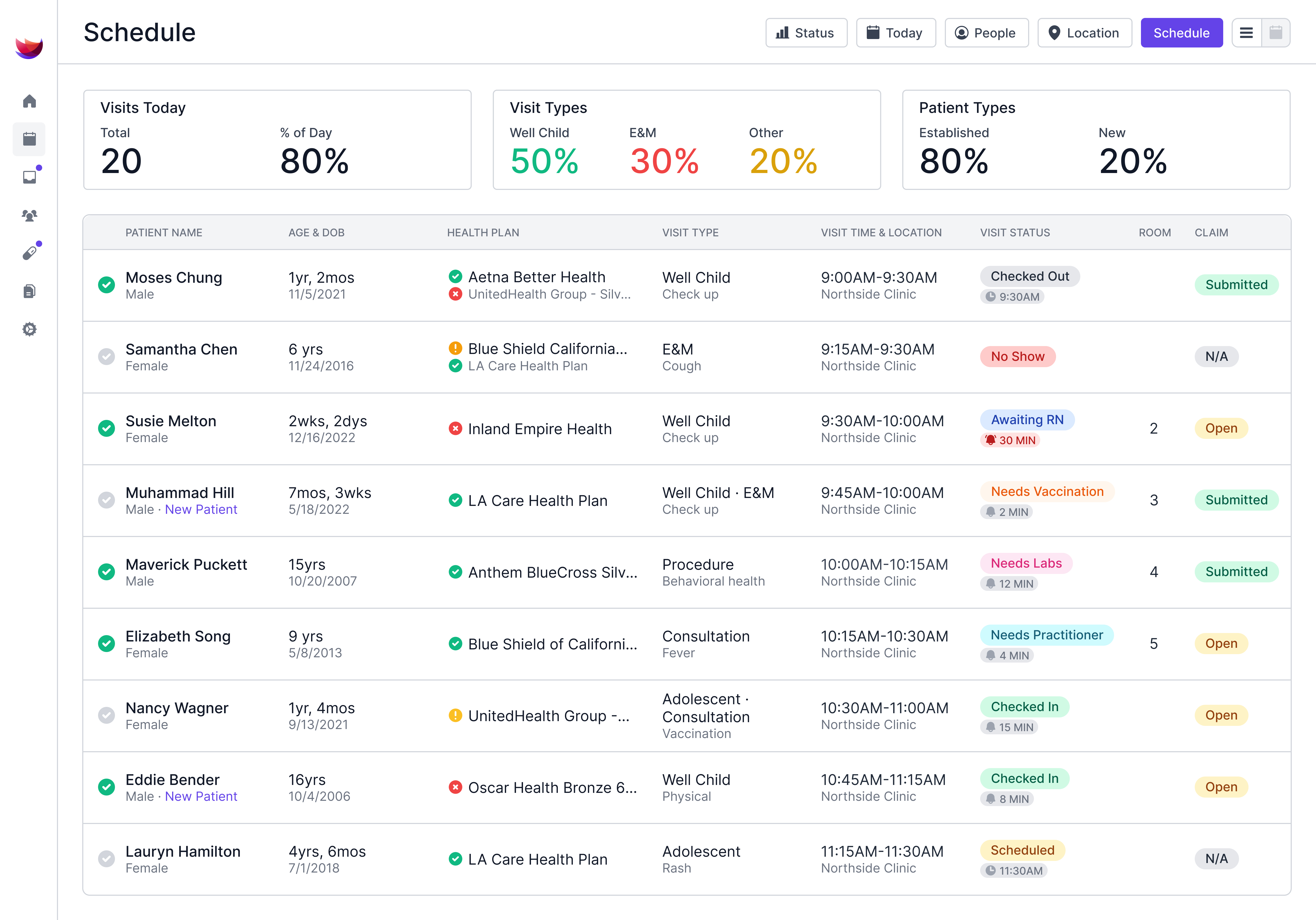
Pediatric billing has more moving parts than most specialties. Between age-based code splits, component-level vaccine billing, and Medicaid-specific rules, even experienced billers lose revenue to avoidable coding mistakes.
This pediatric billing cheat sheet covers CPT codes, ICD-10 diagnosis codes, vaccine administration codes, modifiers, and screening codes that independent pediatric clinics use daily.
Well-Child Visit Codes (Preventive Medicine E/M)
These preventive medicine codes are age-based and split into two groups: new and established patients.
New Patient Preventive Visits
Established Patient Preventive Visits
These codes include the age-appropriate history, exam, anticipatory guidance, counseling, and risk factor reduction performed during the visit. Documentation should reflect all of those components.
Quick billing note: The patient's age on the date of service determines the code, not the age at the time of scheduling. A child who turns 5 between booking and the actual visit gets billed under the 5 to 11 code (99383 or 99393), not the 1 to 4 code.
Sick Visit Codes (Problem-Oriented E/M)
When a child comes in for something other than a well-child check, you bill problem-oriented E/M codes. Since the 2021 E/M changes, code selection is based on medical decision making (MDM) complexity or total time.
New Patient Office Visits
Established Patient Office Visits
99213 and 99214 are the workhorses in most pediatric clinics. A strep throat visit with a rapid test and prescription typically falls under 99213. An asthma exacerbation requiring medication changes, a breathing treatment, and a follow-up plan usually qualifies for 99214.
Quick billing note: If a child comes in for a well-child visit but also presents with a separate problem (ear infection, rash, persistent cough), you can bill the preventive visit code and a problem-oriented E/M code on the same date. Append modifier 25 to the sick visit code.
Documentation must clearly distinguish between the two services.
Vaccine Product Codes
Vaccines require two separate code types on every claim: a product code and an administration code. Missing either one triggers partial or full denial.
Common Pediatric Vaccine Product Codes
Vaccine Administration Codes
Pediatric vaccine administration uses a component-based system for patients 18 years old and younger. Each antigen (component) that prevents a separate disease counts individually.
How component counting works:
A single injection of Pediarix (DTaP-HepB-IPV) contains five antigen components: diphtheria, tetanus, pertussis, hepatitis B, and polio. If the physician counsels the family, you bill 90460 x 1 plus 90461 x 4.
For 90460/90461 to apply, the physician or qualified health care professional must provide face-to-face counseling about risks, benefits, and side effects. Without documented counseling, use 90471/90472 instead.
2026 Immunization Counseling Codes
Starting January 1, 2026, three new time-based CPT codes allow billing for immunization counseling on dates when no vaccine is given:
- 90482 - Immunization counseling (no vaccine given), 3 to 10 minutes
- 90483 - Immunization counseling (no vaccine given), >10 to 20 minutes
- 90484 - Immunization counseling (no vaccine given), >20 minutes
Use 90482–90484 when a physician or other qualified health care professional spends at least 3 minutes counseling a patient/family about immunization(s) and no vaccine is administered that day.
If counseling lasts fewer than 3 minutes, it’s not separately reportable. Medicare doesn’t reimburse these codes (CMS has assigned them status indicator 'I'), so check individual commercial payer policies before billing.
If counseling occurs on the same date as an E/M visit, append modifier 25 to the E/M code.
Note: 90460/90461 are still used when a vaccine is administered with counseling (they are vaccine administration codes, not standalone counseling codes).
Modifier 25 applies to the E/M code, not the counseling code. Only time spent counseling on vaccines that were not administered counts toward the time threshold. Don’t include time already captured under 90460/90461 or 90471/90474 for vaccines that were given at the same visit.
Common Pediatric ICD-10 Diagnosis Codes
ICD-10 codes tell the payer why a service was performed. Pairing the wrong diagnosis with a CPT code is one of the fastest ways to trigger a denial.
Preventive Visit Diagnosis Codes
Use Z00.129 as the primary diagnosis for a standard well-child visit. Link Z23 to each vaccine product code and its matching administration code.
Respiratory Conditions
Ear Conditions
GI and Infectious Conditions
Skin Conditions
Behavioral and Developmental Codes
Newborn and Weight-Related Codes
2025 ICD-10 update for BMI codes: BMI codes (Z68 range) should be assigned only when there is an associated, reportable diagnosis, like obesity, documented by the provider. Don’t assign BMI codes during pregnancy. If values fluctuate during an encounter, assign the code for the most severe value.
Developmental Screening and Mental Health Codes
Pediatric practices bill screening codes separately from the well-child visit when using validated tools.
96110 requires a standardized, validated tool. Common tools include the ASQ-3 (Ages and Stages Questionnaire), M-CHAT-R (Modified Checklist for Autism in Toddlers), and PEDS (Parents' Evaluation of Developmental Status).
96127 covers brief behavioral screens like the PHQ-A for adolescent depression, the Pediatric Symptom Checklist (PSC), and the Vanderbilt ADHD rating scales.
Quick billing note: Many payers allow multiple units of 96110 on the same date if different validated instruments are administered. Check payer-specific policies for unit limits.
Key Modifiers for Pediatric Billing
Modifiers prevent denials when multiple services happen on the same visit.
Modifier 25 is the most critical modifier in pediatric billing.
Whenever a provider addresses a separately identifiable problem during a well-child visit, modifier 25 goes on the problem-oriented E/M code. Without it, the payer treats both services as a single encounter and denies the second code.
Pediatric Billing Cheat Sheet: Medicaid vs. Commercial Insurance
Billing rules differ between Medicaid and commercial payers. This matters in pediatrics because a large percentage of patients carry Medicaid coverage.
Vaccines for Children (VFC) program: Practices that participate in VFC receive vaccines at no cost for Medicaid-eligible children. You bill the administration code but not the product code, or you bill the product at $0, depending on state rules.
VFC rules vary significantly by state, so confirm your specific state's requirements for code selection and modifier use.
7 Common Pediatric Billing Mistakes (and How to Avoid Them)
Even with a pediatric billing cheat sheet nearby, these errors come up repeatedly in pediatric clinics.
- Missing the vaccine administration code: Billing the vaccine product code (e.g., 90700 for DTaP) without the administration code (90460 or 90471) results in partial or full denial. Always submit both.
- Under-counting vaccine components: Combination vaccines contain multiple antigens. Pediarix has five components. Pentacel has five. Vaxelis protects against six diseases. Each additional component beyond the first gets its own 90461 code. Miscounting leaves money on the table.
- Wrong age bracket on preventive visit codes: A 12-year-old billed under 99393 (ages 5 to 11) instead of 99394 (ages 12 to 17) will get denied. Age on the date of service controls the code.
- Forgetting modifier 25 on same-day E/M: When a provider addresses a separate problem during a well-child visit, the sick visit code needs modifier 25. Skipping it means the payer rejects the second charge.
- Mismatching ICD-10 and CPT codes: Linking a preventive CPT code (99391) to a diagnosis for acute illness (J06.9) signals a mismatch. The preventive visit links to Z00.129. The sick visit links to the illness code.
- Using outdated codes: CPT and ICD-10 codes change every year. Billing with a deleted or replaced code triggers an automatic rejection. Review your pediatric billing cheat sheet at least quarterly to stay up to date.
- Skipping documentation for counseling: 90460/90461 require documented face-to-face counseling about vaccine risks, benefits, and side effects. If the note only says "vaccines given," the claim defaults to the lower-paying 90471/90472 codes.
Automate Your Pediatric Billing Cheat Sheet With the Right Software
Keeping track of every CPT code, ICD-10 pairing, and modifier rule on paper works until it doesn’t.
Develo is a modern, web-based EMR built exclusively for independent pediatric clinics. It replaces spreadsheets, paper cheat sheets, and bolt-on billing tools with automated charge capture designed around pediatric workflows.
Here is what Develo does to put this pediatric billing cheat sheet on autopilot:
- AI charge capture reads the visit documentation and applies the correct billing codes automatically, including age-specific E/M codes, diagnosis pairings, and modifiers
- Vaccine administration automation adds the right admin codes (90460-90461 or 90471-90474) based on the patient's age, insurance type, and whether the visit is Medicaid or commercial
- BMI Z-diagnosis code logic automatically appends the correct pediatric BMI code for children ages 2 and older during well-child visits
- Real-time eligibility checks verify insurance coverage before the visit, so your team collects accurate co-pays and catches outdated information that causes denials
- Claims pre-submission checks flag mismatched ICD-10 and CPT pairings, missing modifiers, and incomplete documentation before the claim goes out
- Built-in E/M calculator recommends the correct E/M level based on documented time and MDM fields, so providers stop under-coding
You don’t need a separate billing cheat sheet, a clearinghouse workaround, and three third-party tools to bill pediatric claims correctly. You need one platform that handles charge capture, claims, and payments from check-in to reimbursement.
Book a free demo to see how Develo turns your pediatric billing cheat sheet into automated workflows that catch errors before they cost you revenue.
Frequently Asked Questions
What Is a Pediatric Billing Cheat Sheet?
A pediatric billing cheat sheet is a quick-reference document listing the CPT codes, ICD-10 diagnosis codes, vaccine codes, modifiers, and billing rules that pediatric clinics use most often.
It helps billers, front-desk staff, and providers code accurately without searching through full codebooks during busy clinic days.
What CPT Codes Do Pediatric Clinics Use for Well-Child Visits?
Pediatric well-child visits use preventive medicine E/M codes. New patients use 99381 through 99385, split by age group. Established patients use 99391 through 99395. The patient's age on the date of service determines which code applies.
How Do You Bill Vaccines In a Pediatric Office?
Vaccine billing requires two code types on every claim: the product and the administration code. The product code identifies the specific vaccine (e.g., 90707 for MMR). The administration code covers the work of giving the injection and counseling the family.
For patients under 18, use 90460 for the first component with counseling and 90461 for each additional component. Without documented counseling, use 90471/90472.
Can You Bill a Sick Visit and a Well-Child Visit on the Same Day?
Yes. When a provider addresses a separately identifiable problem during a well-child visit, the practice can bill both the preventive code and a problem-oriented E/M code. The sick visit code must include modifier 25, and the documentation must support both services as distinct encounters.
What Is the Difference Between 90460 and 90471?
The main difference is that 90460 covers vaccine administration with physician counseling about risks, benefits, and side effects. It pays more and applies to patients under 18. 90471 covers vaccine administration without counseling.
If the provider does not document face-to-face counseling, the claim must use 90471 instead of 90460.




.jpg)
%20(1).jpg)
.avif)
.jpg)